Upon arriving at the lab, Claire Joswiak gets ready for a unique day ahead. She walks a couple of buildings over to Lurie Children’s Hospital, gets dressed in scrubs and settles down in a room across from an active operating room. The room is pretty bare bones, with a liquid nitrogen freezer, lab bench, and hood, which she cleans. Now begins the wait.
While Joswiak works on her lab tech responsibilities, like ordering materials and assisting with data analysis on research projects, in the room next door, surgeons are performing what’s called a gonadectomy, a minimally invasive surgery where part of the gonads are removed. For DSD patients, gonadectomies are performed when there is harmful growth, or malignancy, in their gonads. Most commonly, it is a risk of neoplasia, a type of excessive tissue growth, which can lead to gonadal tumors.
Patients at some hospitals, like Lurie Children’s, can also elect to preserve part of their gonadal tissue. This is because reproductive scientists recently discovered that the gonads of some DSD individuals may contain viable germ cells, which suggests fertility potential. While there are currently no means of using the tissue or germ cells for fertility restoration, scientists are actively working to develop techniques to make it possible.
Joswiak said that using research to accelerate potential future fertility opportunities for patients is a key aspect of gonadal tissue cryopreservation.
“I think giving them [patients] the option is probably the most important thing,” she said.
As Joswiak prepares the tissue processing room, she awaits word from the surgeons when the tissue has been extracted. Depending on what kind of tissue they find, such as its size and whether it is more testicular or ovarian, Joswiak begins preparing the tissue to be cryopreserved.
“We can’t really be sure where the germ cells are, whether they are oocytes or spermatogonia. It’s never super obvious,” Joswiak said. While Joswiak prepares half of the tissue, the other half is sent to pathologists to analyze the presence and type of germ cells and detect any malignancies.
The lab, which collaborates with clinicians in the Fertility and Hormone Preservation and Restoration Program and the Supportive Program for a Range of Urogenital Traits, or SPROUT clinic, also receives some information from the medical team before the surgery. Based on clinical indicators, the health team completes a questionnaire about one week before the case, asking them about whether they predict the tissue leans more ovarian or more testicular.
Knowing these characteristics is important because ovarian and testicular tissue are preserved differently. For example, they each require different types of cryopreservation media. Media is a nutrient-rich liquid that the tissue is preserved in to keep it viable during the freezing process.
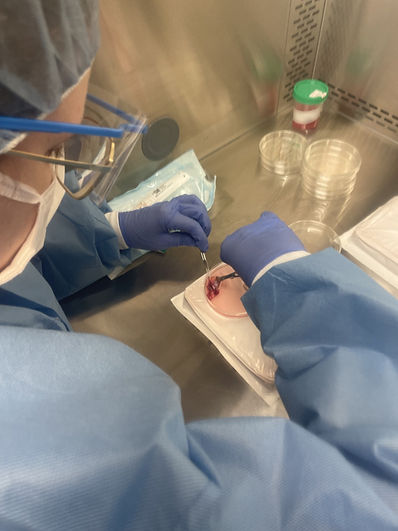
Joswiak follows the lab’s meticulous, standardized protocol for tissue processing. When Joswiak receives the tissue from the surgical team, she first weighs it. She then slices and divides the tissue across different cryopreservation vials with media. This requires detailed labeling and photography to keep track of where each tissue piece comes from.
Noting the orientation of tissue pieces is important because different areas of the gonad contain different types of cells. Also, in cases where the pathologists find malignancies in their half of the tissue sample, the lab has to thaw the other half and send it to them for further analysis. Knowing the anatomical origins of each tissue piece is important for pathologists to be able to identify the location and types of potential malignancies.
The Laronda lab is working on several projects that could allow for the use of this cryopreserved tissue for fertility and hormone restoration options for DSD patients. First, scientists in the lab are working to better understand the types of germ cells, and their surrounding environment, within gonads of DSD patients. DSD encompasses a wide range of differences, so analyzing tissue from a spectrum of patients is key. This could help identify trends across gonads of individuals with similar DSD diagnoses.
The lab’s next step is to develop restoration technologies that would allow maturing follicles, the sacs of cells that secrete hormones and hold maturing eggs, and sperm in the lab using germ cells from preserved tissue. These techniques could also be used to derive hormone-producing cells from patient tissue.
While the fertility potential of tissue obtained from gonadectomy can vary based on the presence of absence of germ cells, researchers in the Laronda lab are hopeful that their work will accelerate research that could provide patients with options in the future. Principal investigator Dr. Monica Laronda reflected on what the establishment of such fertility restoration technologies would mean for individuals with DSD.
“If we are able to make discoveries that enable DSD patients to utilize germ cells from their tissue, then we have preserved this tissue for them. Our patients would then have an option that they would not have otherwise had to pursue having biological children when they become adults,” she said.